By ANISH KOKA
I used to be listening to a dialog between two important thinkers I respect drastically: geneticist/technologist/blogger Razib Khan and Washington Put up columnist Megan McArdle. Their dialogue was a freewheeling rant concerning the issues they see with the rise of populism on the left and proper, however a throwaway remark associated to the US doctor scarcity within the context of needing excessive expert immigrant labor in direction of the tip of the just about two-hour dialog made me notice how little folks actually find out about healthcare in America. After all, everybody is aware of sure points of healthcare as a client very nicely, however even in case you are a high-IQ particular person who could make use of the huge data in any respect of our fingertips, it’s laborious to actually know what the fact on the bottom is with out residing it / having deep data. Curiously sufficient, early on Megan and Razib each acknowledge the impossibility of commenting on the state of affairs in Iran, as a result of the Iraq battle taught them the folly of creating conclusions from the obtainable data. Backside line, it doesn’t matter how good you’re in case your conclusions are based mostly on studying Colin Powell on the weapons of mass destruction Saddam Hussein will need to have. The general public might not notice it, however well being coverage has an identical drawback. The overwhelming majority of lecturers “protecting” American well being coverage, and accountable for describing healthcare, are ideologues whose important aim is to not describe actuality, however to vogue a narrative. And as any screenwriter will let you know — don’t let the information get in the way in which of a great story.
What follows is an examination of what occurs once you pull one of many essential healthcare threads that varieties the bedrock of many healthcare opinions that good folks like Megan and Razib maintain: Rural entry to healthcare in America.
First, right here’s what a Google search reveals — and spot the sources. I guarantee you that PubMed just isn’t a lot totally different. Rural healthcare entry in America should be dangerous, proper?
As soon as we set up that healthcare entry in rural America is “dangerous”, there are all types of conclusions which might be downstream from that like funding of rural hospitals, and administration of the doctor labor provide.
However the unusual factor concerning the rural healthcare entry drawback that ought to strike anybody over a sure age that has adopted/lived healthcare is that we’ve been speaking about this and passing laws on the matter perpetually, and but in case you are to consider those that ought to have essentially the most data about these items, we proceed to fall quick.
Understanding what precisely is going on requires some data of the legislative sausage that has created the present panorama. Understanding the legal guidelines and extra importantly how they’re applied ought to rapidly make the reader perceive why there’s a highly effective incentive to keep up a sure narrative.
A short abstract of some main laws presently on the books exposes precisely why it might be so essential to keep up a sure narrative on rural well being care entry.
The Crucial Entry Hospital (CAH) designation, created by the Balanced Price range Act of 1997 after a wave of rural closures, gave over 1,300 hospitals cost-based Medicare reimbursement — which means Medicare pays regardless of the hospital reviews it price to ship the service.
The Rural Well being Care Entry Act of 2025 (H.R. 771) goes additional, eliminating the space requirement {that a} hospital should be greater than 35 miles from one other hospital to qualify as a CAH, extending cost-based reimbursement to hospitals that had been by no means distant sufficient to satisfy the unique threshold.
The Rural Emergency Hospital (REH) designation permits low-volume rural hospitals to drop inpatient beds whereas retaining emergency and outpatient providers — and receiving extra federal funds — with current laws proposing to increase eligibility to hospitals that closed way back to 2014.
Congress has additionally allotted new Medicare-funded Graduate Medical Schooling (GME) residency slots particularly for rural hospitals, regardless that a December 2025 GAO report discovered that 95 % of the hospitals receiving slots had been geographically city hospitals that had legally reclassified themselves as rural to qualify.
The Rural Well being Focus Act formally authorizes the CDC Workplace of Rural Well being with devoted appropriations, and the Truthful Funding for Rural Hospitals Act modernizes disproportionate share hospital funds with a $20 million per-state funding ground.
Maybe most consequentially, one of many main political shields towards site-neutral cost reform — the coverage that might equalize Medicare reimbursement no matter whether or not a service is delivered in a hospital outpatient division or a doctor’s workplace — a change that might save Medicare tens of billions yearly comes from these arguing that this alteration would shut a whole lot of rural hospitals inside six months.
Each one in every of these packages represents a funding line. And each try to shut the loopholes in these packages is rapidly crushed with an avalanche of moralizing about saving cash on the again of the indigent. You possibly can perceive that there are a whole lot of pursuits which have a lot to realize by promulgating a rural well being care entry hole. Nowhere is the spin on American healthcare extra apparent than when it falls to lecturers to critique it. Educational well being coverage wonks nationally and internationally persistently rank American healthcare as woefully insufficient relative to our peer nations which have some type of nationalized/socialized healthcare.
This narrative has a strong institutional house. The Commonwealth Fund’s Mirror Mirror report, in all probability essentially the most extensively cited worldwide healthcare comparability, has ranked the US final or near-last amongst high-income international locations in nearly each version for the previous 20 years. The report’s methodology leans closely on insurance coverage protection, administrative burden, fairness metrics, and survey-based measures of affected person expertise. Nations with nationwide insurance coverage techniques — the UK, Canada, and the Nordic international locations — rating nicely on the entry dimension nearly by definition, as a result of common protection is handled as equal to common entry. The American system, with its patchwork of personal insurance coverage, Medicaid, and Medicare performs poorly on these metrics and will get ranked accordingly. These rankings are then cited in congressional testimony, think-tank reviews, and op-ed pages as proof that the American healthcare system is inferior — that Individuals get much less for extra, and {that a} nationwide insurance coverage program would repair it.
However what good is a nationwide insurance coverage card if there isn’t any hospital inside the important 90 minute time window when you’ve got a coronary heart assault? Insurance coverage protection and geographic entry to care are usually not the identical factor. A affected person in rural Canada has common protection however might wait hours for an ambulance to achieve a cardiac cath lab — if one is reachable in any respect. A affected person in rural Nevada could also be uninsured and be at a PCI-capable hospital in 40 minutes. The previous is counted as “entry” within the Commonwealth Fund framework. The latter is counted as a failure. The rankings measure the bureaucratic structure of insurance coverage techniques, not the bodily actuality of whether or not care might be delivered, particularly when it’s most urgently wanted.
So how about we really attempt to quantify the American patchwork and evaluate it to one in every of our peer nations that’s imagined to be a mannequin for us — our Medicare for All Canadian neighbor.
Percutaneous coronary intervention — the process that opens a blocked coronary artery throughout a coronary heart assault — is near a great proxy for healthcare entry broadly. It’s definitionally time-sensitive: the ACC/AHA pointers set a 90-minute door-to-balloon goal for a motive, and delays past that threshold carry measurable mortality/morbidity penalties. It requires important infrastructure — a catheterization laboratory, educated interventional cardiologists, a specialised workforce obtainable across the clock. It’s due to this fact not uniformly distributed throughout geographies. And crucially, it’s a process the place we’ve wonderful public knowledge on precisely the place it’s being carried out.
Entry to PCI just isn’t an ideal proxy for entry to all medical care. But when a neighborhood has a functioning PCI program inside affordable distance, it nearly definitely has the broader infrastructure — emergency providers, hospital beds, superior imaging, specialist protection — that defines a practical healthcare ecosystem. The inverse can also be roughly true: communities removed from PCI are usually removed from the remainder of superior care as nicely. PCI entry is an inexpensive healthcare canary.
Once you measure the precise distance between the place Individuals reside and the place the closest cath lab is — utilizing actual hospital knowledge and population-weighted geography — what do we discover?
Constructing the maps — and what they present
How the U.S. map was constructed
The inspiration is a 2006 paper by Nallamothu et al. in Circulation — nonetheless essentially the most rigorous printed evaluation of geographic PCI entry in the US — which discovered that 84% of Individuals reside inside 60 minutes of a PCI-capable hospital. Utilizing Medicare billing data for DRG codes 246–251 to establish 1,322 hospitals actively performing PCI, and replicating the Nallamothu methodology with up to date knowledge, I discover basically the identical outcome. No comparable developed nation approaches this stage of entry — and I’ll get to what the closest peer comparisons really appear like under.
However a easy county choropleth — coloration every county by drive time — has a basic drawback: it treats a county of 600 folks identically to one in every of 600,000. The huge empty counties of the inside West look alarming on the map, and their sheer geographic mass dominates the visible.
The policy-relevant query just isn’t which counties are removed from PCI, however whether or not the individuals who reside in these counties are removed from PCI — and whether or not the inhabitants density in these areas justifies the type of infrastructure funding the agricultural entry narrative requires.
To reply the query I constructed a bivariate map encoding each dimensions, inhabitants density, and distance to a PCI-capable hospital. Counties are assigned to a few density classes utilizing the fiftieth and ninetieth percentiles of the county density distribution — percentile-based thresholds slightly than arbitrary absolute cutoffs.
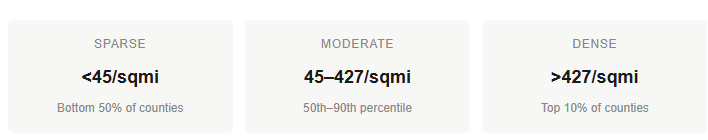
I then outlined three entry bands anchored to the ACC/AHA guideline for opening a blocked artery within the setting of an acute coronary heart assault: inside half-hour, 30 to 90 minutes, and past 90 minutes. Past 90 minutes is a vital threshold that defines the purpose the place most people can have a cardiac scar or worse if they’re exterior this time window for artery opening.

The centroid drawback — and why it issues
Making a database of drive time from a hospital requires defining the place to measure from. The USA is separated into counties, and taking the geographic middle of the county (the geographic centroid) as the space to measure from creates some meaningless distortions as a result of the inhabitants in any given county just isn’t essentially clustered in the midst of the county. Giant western counties the place almost all of the inhabitants is clustered in a single nook of an enormous space clarify why the straightforward geographic centroid fails so badly.
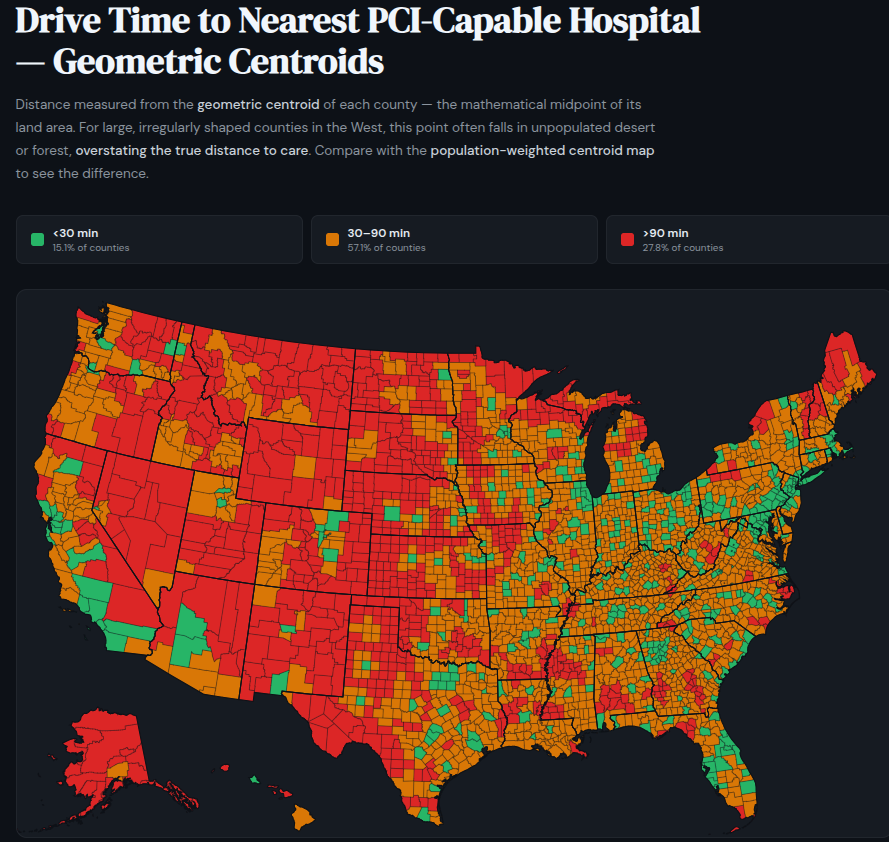
Click on on the map to be taken to an interactive map
Reno sits within the southwest nook of Washoe County, house to Renown Regional Medical Middle and St. Mary’s Regional. However Washoe County extends a whole lot of miles into the Nevada desert. Its geometric centroid lands 43.5 miles from Renown, in an space the place basically no one lives — and an earlier model of a map I made marked it crimson. Fortunately, the Census Bureau publishes population-weighted centroids for all 3,143 U.S. counties within the CenPop2020 file, calculated from 2020 block-level knowledge. Washoe’s population-weighted centroid is 3.8 miles from Renown. That’s the right quantity, and so I used population-weighted centroids for each U.S. county.

What the U.S. map really reveals
The hanging discovering just isn’t about dense counties — dense counties cluster round cities, and cities have hospitals. The hanging discovering is concerning the reasonable and sparse counties: even at low inhabitants densities, a surprisingly giant share of the American inhabitants is inside the 90-minute guideline window. However regardless of the big federal equipment devoted to rural healthcare entry, 2.2 million Individuals in moderate-density counties and 9.5 million in sparse counties — roughly 11.7 million whole, or about 3.5% of the inhabitants — reside past 90 minutes from a PCI hospital. These are the folks the agricultural entry laws is ostensibly constructed for, and after a long time of CAH designations, GME slot carve-outs, Rural Emergency Hospital packages, and billions in cost-based reimbursement, that’s what stays.
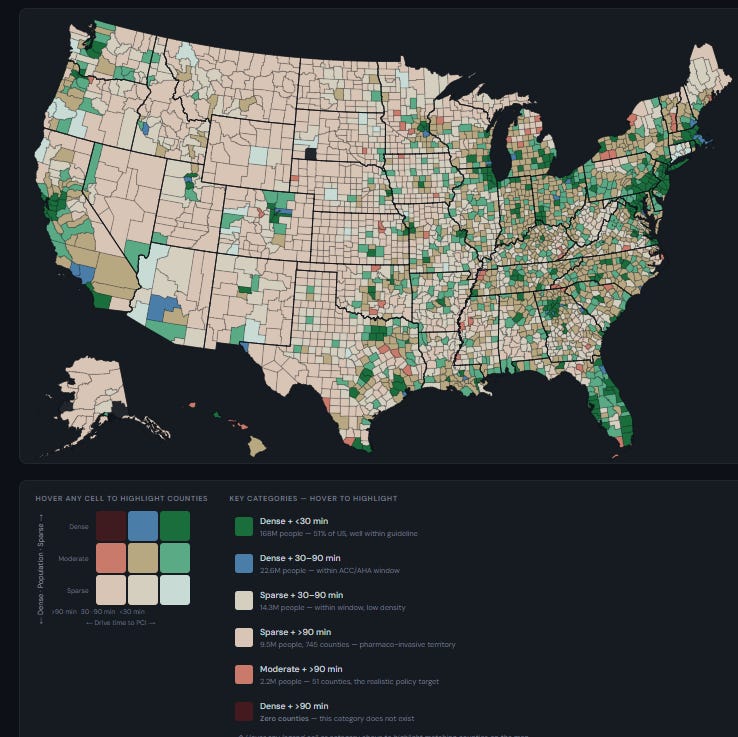
Click on on the map for an interactive model
The peer comparability drawback — the U.S. is genuinely with out friends
Each worldwide comparability of healthcare entry implicitly assumes the international locations being in contrast are meaningfully comparable. They don’t seem to be — at the least not for this query. The USA is the third-largest nation on this planet by land space and the third most populous. No high-income democracy comes near combining each. The UK has 68 million folks in an space smaller than Oregon. The Nordic international locations collectively have fewer folks than the larger New York metropolitan space unfold throughout a landmass that’s largely accessible by street. These international locations face no significant analog to the American geographic entry drawback.
The international locations that do approximate the U.S. in scale — Russia, China, India, Brazil — fail so comprehensively on PCI entry that no significant comparability is feasible. Russia has maybe 100 PCI facilities for 144 million folks throughout 11 time zones. China’s cath lab infrastructure is closely concentrated in coastal cities. India and Brazil have dramatic urban-rural gradients at a severity that makes rural Nevada look well-served. These are usually not peer comparators. They’re cautionary tales about what really occurs when healthcare infrastructure is inadequate at continental scale.
This is the reason worldwide entry rankings that place the US alongside Belgium, the Netherlands, and New Zealand are usually not measuring the identical factor. A rustic the dimensions of Maryland with common insurance coverage and three PCI facilities serving a compact inhabitants just isn’t navigating the identical entry problem as a rustic spanning 4 time zones with 335 million folks. The Commonwealth Fund framework doesn’t account for this, however the bivariate maps do.
Canada: the closest reputable comparability — and a sobering one
Canada is essentially the most defensible peer comparability — related authorized and institutional custom, related earnings stage, bodily adjoining, and steadily invoked by American reform advocates as a mannequin. However making the Canadian map concerned totally different decisions than the U.S. map.
The Canadian map makes use of census divisions slightly than counties — there are 282 of them, in comparison with 3,143 U.S. counties. PCI middle areas had been compiled from CIHI Cardiac Care High quality Indicators and provincial cardiac community directories slightly than from a Medicare billing equal, as a result of Canada has no public analog to the CMS procedure-level knowledge. The 30 facilities recognized are the very best obtainable depend, however the sourcing is much less rigorous than the U.S. strategy.
Extra importantly, the density thresholds for Canada are calculated individually from Canadian census division percentiles — sparse under 17 per sq. mile, reasonable 17 to 213, dense above 213 — slightly than making use of U.S. thresholds. Canada is simply so darn sparsely populated total that making use of U.S. density thresholds would classify nearly each Canadian census division as sparse, collapsing the bivariate evaluation right into a single meaningless class. Even with Canada-specific thresholds which might be much more forgiving than U.S. ones (what counts as “dense” in Canada can be “reasonable” in the US) the comparability remains to be stark.
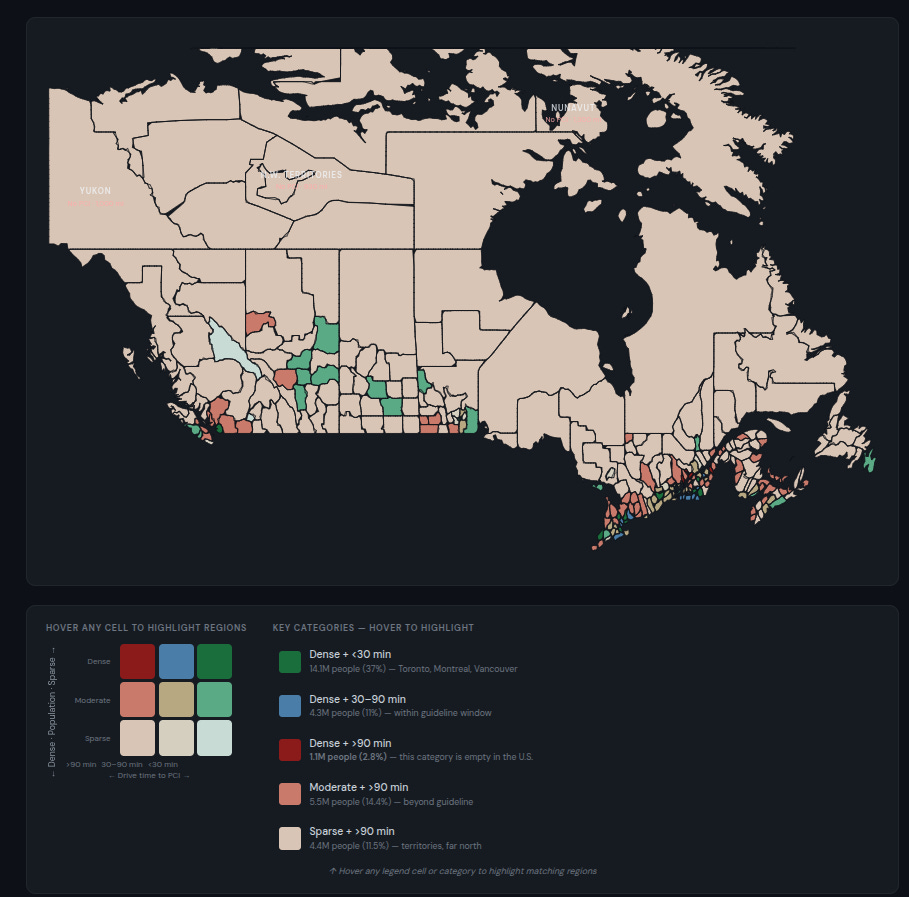
Baber et al. in Open Drugs (2011) discovered that 63.9% of Canadians aged 40 and older reside inside 60 minutes of a PCI facility, versus 84% of Individuals. That 20-point hole displays a rustic the place 30 PCI facilities serve 38 million folks unfold the world over’s second-largest landmass, concentrated nearly completely inside 125 miles of the U.S. border. Making use of the identical bivariate methodology, roughly 10.9 million Canadians — 28.7% of the overall inhabitants — reside past 90 minutes from a PCI hospital. That features:
- 4.4 million in sparse census divisions past 90 minutes (11.5% of inhabitants)
- 5.5 million in moderate-density census divisions past 90 minutes (14.4%)
- 1.1 million in dense census divisions past 90 minutes (2.8%) — a class that comprises zero Individuals
These 1.1 million Canadians in dense-but-far census divisions signify the starkest distinction with the US. They’re concentrated within the Quebec Metropolis–Trois-Rivières hall — a populated, accessible stretch of southern Quebec that in any affordable sense ought to be well-served. And but, remarkably, it isn’t.
I manually checked this to ensure the code was right. Listed here are the 4 dense census divisions and their nearest PCI hospitals:
- Francheville (Trois-Rivières space, 452,604 folks): nearest PCI is the Institut universitaire de cardiologie et de pneumologie de Québec — 54.6 miles, estimated 110 minutes
- D’Autray (Berthierville space, 266,948 folks): nearest PCI is the Montreal Coronary heart Institute — 53.4 miles, estimated 108 minutes
- Shawinigan (195,640 folks): nearest PCI is the Institut universitaire de cardiologie — 75.9 miles, estimated 147 minutes
- Montmagny (east of Quebec Metropolis, 150,022 folks): nearest PCI is the Institut universitaire de cardiologie — 47.9 miles, estimated 98 minutes
To place the general numbers in context: the U.S., with almost 9 instances Canada’s inhabitants, has 11.7 million folks past the 90-minute threshold — 3.5% of its inhabitants. Canada has 10.9 million past the edge out of 38 million — 28.7%. On a per-capita foundation, Canada’s entry hole is roughly eight instances worse than America’s, in a rustic the place 90% of the inhabitants lives in a slender temperate hall alongside the world’s longest undefended border. A easy framing of American rural entry as a disaster that calls for X whereas holding up Canadian Medicare as a mannequin tells me you’re both uninformed or have a canine within the combat.
So the place does this go away us?
The USA just isn’t excellent. Eleven level seven million Individuals reside past the 90-minute window for emergency cardiac care, and that issues. Each a type of folks deserves higher. However the sincere framing of that quantity is that it represents 3.5% of the inhabitants of a continent-spanning nation — and that no comparable nation on earth comes near matching it. Canada, the nation most steadily held up because the mannequin America ought to comply with, leaves 28.7% of its inhabitants exterior that very same window, together with over one million folks in densely populated (by Canada requirements) areas. Rural healthcare entry is a genuinely laborious drawback at continental scale and the headline ought to be that the US has solved extra of that drawback than anybody else.
And but this isn’t the story you’ll learn within the Commonwealth Fund reviews, or within the well being coverage journals, or within the congressional testimony that precedes the following spherical of rural hospital funding. The dominant narrative — that American rural healthcare is in disaster, that we’re falling behind our friends, that the system is failing — is maintained by two teams with aligned incentives. The primary is the tutorial and advocacy class that wishes a government-payer system and desires American healthcare to look damaged to justify the overhaul. The Canadian comparability is instructive: the single-payer system they need Individuals to undertake delivers measurably worse geographic entry to emergency cardiac care than the patchwork they need to exchange. The second group is the healthcare trade itself — the well being techniques, the hospital associations, the directors of residency coaching packages and the hospitals which might be all too completely happy to make the most of a Medicare funded program that offers them free doctor labor. All of that is fueled by funding streams that, partly, depend upon the continued notion of a rural entry disaster. The Crucial Entry Hospital program, the Rural Emergency Hospital designation, the agricultural GME carve-outs: each one in every of these represents cash flowing to establishments, and each try and reform them is met with the identical argument — that any change will shut hospitals and kill sufferers.
The result’s a coverage panorama the place the issue isn’t outlined with actual metrics, the funding isn’t tied to measurable entry outcomes, and the identical establishments that take in billions in rural subsidies additionally foyer aggressively towards significant laws like site-neutral cost reform. Well being techniques swallow huge quantities of federal funding and nonetheless can’t fully shut the remaining entry gaps. (What they’ll do, and do very successfully, is drive up the price of care for everybody else.)
There are a lot of different levers to drag on if we need to be actually distinctive and enhance rural entry for the 11.7 million Individuals who stay comparatively underserved. I hope I’ve satisfied you that the straightforward Canadian choice supplied up by many would take us backwards, not ahead. There are some much more smart choices that ought to have broad public help.
First, it might appear a wiser and a greater long run resolution to unravel the doctor shortage drawback in rural areas by permitting for many who develop up in these communities to journey a vastly accelerated path to turning into a common practitioner. In the mean time a brilliant younger child in rural West Virginia is more likely to run his personal HVAC store than run his personal main care observe. Any present main care practitioner will let you know the HVAC route is a a lot smarter and extra profitable path than a path to turning into a doctor that has you spending a minimal of 11 years after graduating from highschool and accruing mid six figures value of debt. It wasn’t all the time that method — a century in the past, an adolescent may go from highschool to training drugs in 5 or 6 years, and plenty of of these physicians served precisely these sorts of communities. So Megan and Razib’s touch upon doctor shortages and the necessity for prime expert immigrant labor that isn’t doable to be sourced regionally has a whole lot of layers to it. The “scarcity” is partly a operate of funding a whole lot of residency spots in rural areas, which might be then stuffed by abroad physicians on the lookout for an entry level to the US well being care system. This framework is a coverage selection that doesn’t even do a great job of ever fixing the issue as a result of physicians from Lahore and Hyderabad (or their kids, who overwhelmingly go away drugs/ select to observe drugs in metropolitan areas) solely keep in these communities in the event that they haven’t any different choice. If we, for example, stopped funding rural residency slots, these hospitals which might be nonetheless awash in money from a wide range of different federal packages would select totally different labor choices (nurse practitioners/doctor assistants/pay extra to native household observe docs to assist employees sufferers), and abruptly you’d have a really totally different trying panorama of “want” for physicians. Backside line: if you’re going to attempt to engineer one thing — make it extra engaging for native members of the neighborhood to grow to be physicians of their neighborhood slightly than massively incentivizing rural hospitals to import physicians to fill a necessity that you just created.
Second, if we’re to make use of American tax {dollars} to shut the agricultural entry hole, we have to demand higher outcomes. The info exists to measure, county by county, how far Individuals really are from emergency cardiac care, main care, and primary surgical providers. Tie funding to some mixture of these measurements. If a rural well being system is receiving cost-based reimbursement, GME coaching slots, and Rural Emergency Hospital subsidies, it ought to be required to show what entry it’s offering — next-day main care appointments, 24/7 emergency protection, PCI functionality — and lose its designation (and funding) if it can’t.
Third, since we really need extra hospitals, we should always break the monopoly C-suite has on the opening of recent hospitals. The doctor hospital possession ban — a product of the Reasonably priced Care Act, lobbied for by the hospital trade — prevents the folks almost definitely to unravel rural entry issues from doing so. Physicians from rural communities who need to increase capital, construct amenities, and ship care are legally prohibited from proudly owning the hospitals they’d employees. The ban protects incumbent well being techniques from competitors. It does nothing for sufferers. Think about what occurs the place physicians can personal amenities: Atlas Surgical procedure Middle in Amherst, New York — a physician-owned ambulatory surgical procedure middle constructed by the neurosurgeons of College at Buffalo Neurosurgery — performs same-day awake endovascular neurosurgery, carotid stenting, Gamma Knife radiosurgery, and sophisticated backbone procedures that might in any other case require multi-day hospital admissions at far larger price. It’s the first ambulatory middle within the nation to supply outpatient Gamma Knife. That’s what doctor possession produces when the legislation permits it. Now think about that mannequin utilized to rural communities that want a hospital and have physicians prepared to construct one. Presently, the legislation says no.
Your entire rural entry debate is premised on the idea that solely giant well being techniques backed by federal subsidies can ship care in underserved areas. The proof for that is skinny. What the proof really reveals is that when physicians are allowed to personal and function amenities — ambulatory surgical procedure facilities, imaging facilities, pressing care networks — they ship care at decrease price with comparable or higher outcomes. Extending that mannequin to hospital possession in underserved areas is essentially the most direct path to closing the remaining entry gaps with out the perpetual subsidy machine that has manifestly failed to shut them over three a long time.
The mountain to climb is excessive. Step one stands out as the hardest: reducing by way of the noise of motivated lecturers who management many of the messaging on well being coverage and healthcare entry. The general public ought to have a transparent understanding that the disaster narrative they’ve been offered just isn’t an outline of actuality however a product — manufactured by those that revenue from it, whether or not in funding or in political capital. Ought to we attempt to do it even higher? After all.
However there may be little hope of getting wherever and not using a good grasp of the scope of the issue that faces us.
Anish Koka is a Heart specialist in Philadelphia. He writes on drugs and well being coverage on his substack the place this was initially printed and in addition cohosts a weekly podcast : The Docs Lounge
Hyperlink to PCI entry US/Canada Interactive maps | Extra on map methodology, limitations

